21 results
Emergency Department Admission Rates, Waiting Times, and Mortality: An Observational Study in the Tertiary Center Most Proximal to Gaza During a Military Conflict
- Jacob Dreiher, Sharon Einav, Shlomi Codish, Amit Frenkel
-
- Journal:
- Disaster Medicine and Public Health Preparedness / Volume 17 / 2023
- Published online by Cambridge University Press:
- 23 August 2023, e463
-
- Article
- Export citation
-
Objectives:
Military conflicts may be ongoing and encompass multiple medical facilities. This study investigated the impact of a military conflict (“Protective Edge” PE) on emergency department (ED) function in a tertiary medical center.
Methods:Visits to the ED during PE (July-August 2014) were compared with ED visits during July-August 2013 and 2015 with regard to admission rates, waiting times and 30-d mortality. Odds ratios (ORs) adjusted for confounders were used for the multivariable regression models.
Results:There were 32,343 visits during PE and 74,279 visits during the comparison periods. A 13% decrease in the daily number of visits was noted. During PE, longer waiting times were found, on average 0.25 h longer, controlling for confounders. The difference in waiting times was greater in medicine and surgery. Admission rates were on average 10% higher during PE military conflict, controlling for confounders. This difference decreased to 7% controlling for the daily number of visits. Thirty-day mortality was significantly increased during PE (OR = 1.42; 95% CI: 1.18-1.70). ORs for mortality during PE were significantly higher in medicine (OR = 1.45; 95% CI: 1.15-1.81) and pediatrics (OR = 4.40; 95% CI: 1.33-14.5).
Conclusions:During an ongoing military conflict, waiting times, admission rates, and mortality were statistically significantly increased.
Tier-based antimicrobial stewardship metrics for genitourinary-related antibiotic use in Veterans’ Affairs outpatient settings
- Matthew Samore, Matthew Goetz, McKenna Nevers, Jacob Crook, Suzette Rovelsky, Ben Brintz, Kelly Echevarria, Melinda Neuhauser, Sharon Tsay, Lauri Hicks, Karl Madaras-Kelly
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue S1 / July 2022
- Published online by Cambridge University Press:
- 16 May 2022, pp. s5-s6
-
- Article
-
- You have access Access
- Open access
- Export citation
-
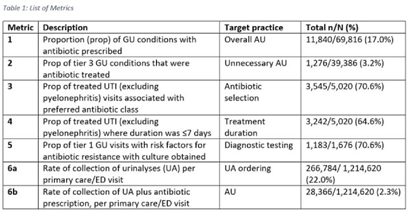
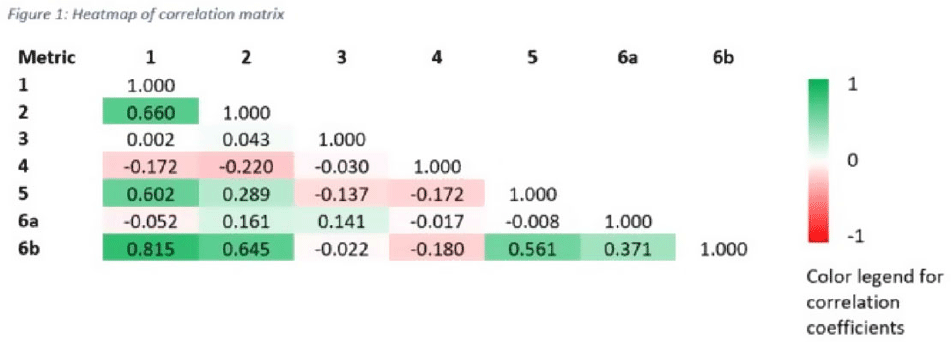
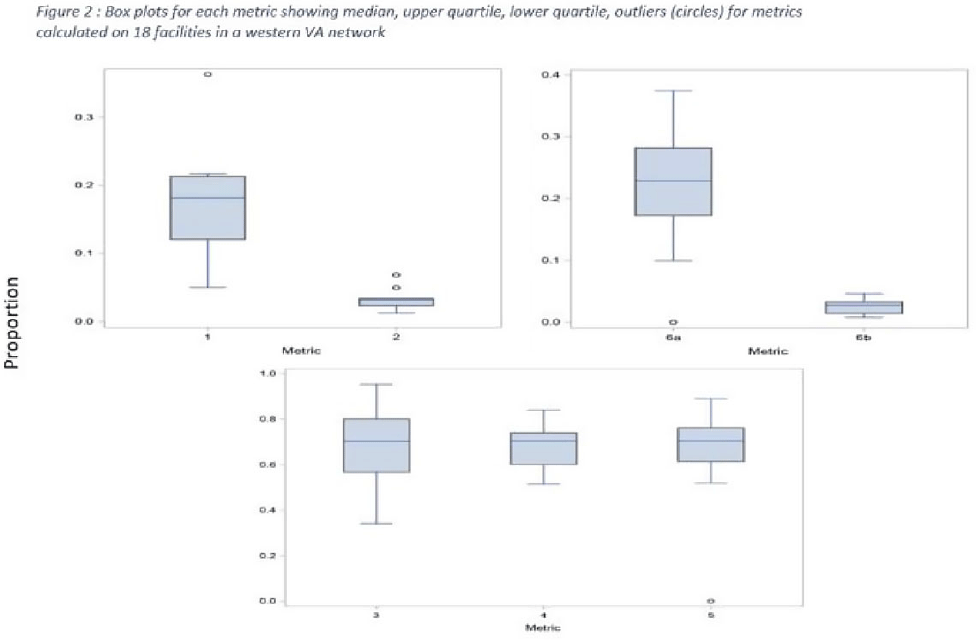
Background: Tracking antibiotic use is a core element of antimicrobial stewardship. We developed a set of metrics based on electronic health record data to support an outpatient stewardship initiative to improve management of urinary tract infections (UTIs) in Veterans’ Affairs (VA) emergency departments (EDs) and primary care clinics. Because UTI diagnostic codes only capture a portion of genitourinary (GU)-related antibiotic use, a tier-based approach was used to evaluate practices. Methods: Metrics were developed to target practices related to antibiotic prescribing and diagnostic testing (Table 1). GU conditions were divided into 3 categories: tier 1, conditions for which antibiotics are usually or always indicated; tier 2, conditions for which antibiotics are sometimes indicated; and tier 3, conditions for which antibiotics are rarely or never indicated (eg, benign prostatic hypertrophy with symptoms). Patients with visits related to urological procedures, nontarget providers, and concomitant non-GU infections were excluded. Descriptive analyses included calculation of the correlation matrix for the 7 metrics and the construction of box plots to display interfacility variability. Results: Metrics were calculated quarterly for 18 VA medical centers, including affiliated clinics, in a western VA network, from July 2018 to June 2020 (Table 1). Tier 3 GU conditions accounted for 1,276 of 11,840 (11%) of GU-related antibiotic use. Metrics 1 and 6b were strongly correlated with each other and were also positively correlated with metrics 2 and 5 (coefficients > 0.5) (Fig. 1). Substantial interfacility variation was observed (Fig. 2). Conclusions: Stewardship metrics for suspected or documented UTIs can identify opportunities for practice improvement. Broadly capturing GU conditions in addition to UTIs may enhance utility for performance feedback. Antibiotic prescribing for tier 3 GU conditions is analogous to unnecessary antibiotic use for acute, uncomplicated bronchitis and upper respiratory tract infections.
Funding: None
Disclosures: None
Capabilities of global high-level isolation units: A pre-workshop survey
- Jocelyn J. Herstein, Timo Wolf, Emanuele Nicastri, Yee Sin Leo, Poh Lian Lim, Michael Jacobs, Sharon Vanairsdale, Eric Toner, Matthew P. Shearer, Angela Vasa, Vikram Mukherjee, Andrea Echeverri, Erica S. Shenoy, John J. Lowe
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 43 / Issue 11 / November 2022
- Published online by Cambridge University Press:
- 01 December 2021, pp. 1679-1685
- Print publication:
- November 2022
-
- Article
- Export citation
-
Objective:
To assess experience, physical infrastructure, and capabilities of high-level isolation units (HLIUs) planning to participate in a 2018 global HLIU workshop hosted by the US National Emerging Special Pathogens Training and Education Center (NETEC).
Design:An electronic survey elicited information on general HLIU organization, operating costs, staffing models, and infection control protocols of select global units.
Setting and participants:The survey was distributed to site representatives of 22 HLIUs located in the United States, Europe, and Asia; 19 (86%) responded.
Methods:Data were coded and analyzed using descriptive statistics.
Results:The mean annual reported budget for the 19 responding units was US$484,615. Most (89%) had treated a suspected or confirmed case of a high-consequence infectious disease. Reported composition of trained teams included a broad range of clinical and nonclinical roles. The mean number of HLIU beds was 6.37 (median, 4; range, 2–20) for adults and 4.23 (median, 2; range, 1–10) for children; however, capacity was dependent on pathogen.
Conclusions:Responding HLIUs represent some of the most experienced HLIUs in the world. Variation in reported unit infrastructure, capabilities, and procedures demonstrate the variety of HLIU approaches. A number of technical questions unique to HLIUs remain unanswered related to physical design, infection prevention and control procedures, and staffing and training. These key areas represent potential focal points for future evidence and practice guidelines. These data are important considerations for hospitals considering the design and development of HLIUs, and there is a need for continued global HLIU collaboration to define best practices.
A Change from a Spinal Immobilization to a Spinal Motion Restriction Protocol was Not Associated with an Increase in Disabling Spinal Cord Injuries
- Brian M. Clemency, Peter Natalzia, Johanna Innes, Sharon Guarino, Jacob V. Welch, Arsalan Haghdel, Ekaterina Noyes, Jeffery Jordan, Heather A. Lindstrom, E. Brooke Lerner
-
- Journal:
- Prehospital and Disaster Medicine / Volume 36 / Issue 6 / December 2021
- Published online by Cambridge University Press:
- 03 November 2021, pp. 708-712
- Print publication:
- December 2021
-
- Article
- Export citation
-
Background:
Over the past decade, Emergency Medical Service (EMS) systems decreased backboard use as they transition from spinal immobilization (SI) protocols to spinal motion restriction (SMR) protocols. Since this change, no study has examined its effect on the neurologic outcomes of patients with spine injuries.
Objectives:The object of this study is to determine if a state-wide protocol change from an SI to an SMR protocol had an effect on the incidence of disabling spinal cord injuries.
Methods:This was a retrospective review of patients in a single Level I trauma center before and after a change in spinal injury protocols. A two-step review of the record was used to classify spinal cord injuries as disabling or not disabling. A binary logistic regression was used to determine the effects of protocol, gender, age, level of injury, and mechanism of injury (MOI) on the incidence of significant disability from a spinal cord injury.
Results:A total of 549 patients in the SI period and 623 patients in the SMR period were included in the analysis. In the logistic regression, the change from an SI protocol to an SMR protocol did not demonstrate a significant effect on the incidence of disabling spinal injuries (OR: 0.78; 95% CI, 0.44 - 1.36).
Conclusion:This study did not demonstrate an increase in disabling spinal cord injuries after a shift from an SI protocol to an SMR protocol. This finding, in addition to existing literature, supports the introduction of SMR protocols and the decreased use of the backboard.
What mental health professionals and organisations should do to address climate change
- Part of
- Adam Monsell, Jacob Krzanowski, Lisa Page, Sharon Cuthbert, Guy Harvey
-
- Journal:
- BJPsych Bulletin / Volume 45 / Issue 4 / August 2021
- Published online by Cambridge University Press:
- 05 May 2021, pp. 215-221
- Print publication:
- August 2021
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Aims and method
The climate change emergency is also a mental healthcare emergency. We seek to provide a framework for what mental health professionals and organisations should do to make their practice more sustainable.
ResultsThere are ethical, legal and organisational imperatives to make mental healthcare more sustainable. Mental healthcare must be refocused with an emphasis on prevention, building social capital and community resilience. Patients must be empowered to manage their own mental health. Efficiencies should be found within the system. Low-carbon ways to deliver care must be found, measured and improved upon. Greater adaptability needs to be built into the system to mitigate the impact of climate change. Sustainability should be integrated into training programmes, and good examples of practice shared and celebrated.
Clinical implicationsMental health organisations and individuals must act now to prevent and adapt for the climate and ecological emergency. Sustainable practice is also good practice.
Predicting the emergence of full-threshold bipolar I, bipolar II and psychotic disorders in young people presenting to early intervention mental health services
- Joanne S. Carpenter, Jan Scott, Frank Iorfino, Jacob J. Crouse, Nicholas Ho, Daniel F. Hermens, Shane P. M. Cross, Sharon L. Naismith, Adam J. Guastella, Elizabeth M. Scott, Ian B. Hickie
-
- Journal:
- Psychological Medicine / Volume 52 / Issue 10 / July 2022
- Published online by Cambridge University Press:
- 30 October 2020, pp. 1990-2000
-
- Article
- Export citation
-
Background
Predictors of new-onset bipolar disorder (BD) or psychotic disorder (PD) have been proposed on the basis of retrospective or prospective studies of ‘at-risk’ cohorts. Few studies have compared concurrently or longitudinally factors associated with the onset of BD or PDs in youth presenting to early intervention services. We aimed to identify clinical predictors of the onset of full-threshold (FT) BD or PD in this population.
MethodMulti-state Markov modelling was used to assess the relationships between baseline characteristics and the likelihood of the onset of FT BD or PD in youth (aged 12–30) presenting to mental health services.
ResultsOf 2330 individuals assessed longitudinally, 4.3% (n = 100) met criteria for new-onset FT BD and 2.2% (n = 51) met criteria for a new-onset FT PD. The emergence of FT BD was associated with older age, lower social and occupational functioning, mania-like experiences (MLE), suicide attempts, reduced incidence of physical illness, childhood-onset depression, and childhood-onset anxiety. The emergence of a PD was associated with older age, male sex, psychosis-like experiences (PLE), suicide attempts, stimulant use, and childhood-onset depression.
ConclusionsIdentifying risk factors for the onset of either BD or PDs in young people presenting to early intervention services is assisted not only by the increased focus on MLE and PLE, but also by recognising the predictive significance of poorer social function, childhood-onset anxiety and mood disorders, and suicide attempts prior to the time of entry to services. Secondary prevention may be enhanced by greater attention to those risk factors that are modifiable or shared by both illness trajectories.
4539 Building a Translational Science pipeline: The Indiana CTSI STEM K-12 Program
- Elmer Sanders, Vanessa Barth, Leigh-Ann Cruz, Ilesha Sherrer, Jacob Olson, Emily Speidell, Elvia Solis, Sharon Harrison, Amy Hinshaw, James A. McAteer
-
- Journal:
- Journal of Clinical and Translational Science / Volume 4 / Issue s1 / June 2020
- Published online by Cambridge University Press:
- 29 July 2020, pp. 57-58
-
- Article
-
- You have access Access
- Open access
- Export citation
-
OBJECTIVES/GOALS:
Develop strong network of science teachers interested in promoting scientific research to their students.
Place students in an immersive summer research internship that, when possible, matches their career interests.
Expose students to the numerous career paths within the STEM field.
METHODS/STUDY POPULATION:
The program recruits socio-economically disadvantaged students and provides them a stipend, and also accepts students who can participate unpaid.
Local school teachers are engaged in a summer fellowship to learn biotechnologies and research. In Spring these teachers help recruit students and during the subsequent Fall help students with college and scholarship applications.
Students are placed in a variety of laboratories within the Schools of Medicine, Science, Dentistry, Public Health, Informatics, Health and Human Sciences, Engineering and Technology, especially in biomedical engineering. Students are also placed in industry laboratories such as Eli Lilly and the Indiana Bioscience Research Institute.
Long-term program follow-up is done through post-internship surveys to assess impact on graduate and professional school admission.
RESULTS/ANTICIPATED RESULTS:
Since the Indiana CTSI was established in 2008, 872 students have participated in the summer internship.
71% of past interns are underrepresented minorities in science or classified as disadvantaged by NIH criteria.
17% of students interned during grade 10, 72% during grade 11, and 11% during grade 12.
21% of students engage in the program for more than one year.
100% of past interns are currently enrolled in or have graduated college.
Over 60% of those with a bachelors degree proceed to graduate and professional schools and over 80% stay in STEM related fields. These rates are equal for interns from underrepresented minorities or those classified as disadvantaged by NIH criteria.
DISCUSSION/SIGNIFICANCE OF IMPACT:
Students engaged in the Indiana CTSI STEM program are progressing through the translational science pipeline based on their graduating from college and remaining in the STEM field.
Transdiagnostic neurocognitive subgroups and functional course in young people with emerging mental disorders: a cohort study
- Jacob J. Crouse, Kate M. Chitty, Frank Iorfino, Joanne S. Carpenter, Django White, Alissa Nichles, Natalia Zmicerevska, Ashleigh M. Tickell, Rico S.C. Lee, Sharon L. Naismith, Elizabeth M. Scott, Jan Scott, Daniel F. Hermens, Ian B. Hickie
-
- Journal:
- BJPsych Open / Volume 6 / Issue 2 / March 2020
- Published online by Cambridge University Press:
- 19 March 2020, e31
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background
Neurocognitive impairments robustly predict functional outcome. However, heterogeneity in neurocognition is common within diagnostic groups, and data-driven analyses reveal homogeneous neurocognitive subgroups cutting across diagnostic boundaries.
AimsTo determine whether data-driven neurocognitive subgroups of young people with emerging mental disorders are associated with 3-year functional course.
MethodModel-based cluster analysis was applied to neurocognitive test scores across nine domains from 629 young people accessing mental health clinics. Cluster groups were compared on demographic, clinical and substance-use measures. Mixed-effects models explored associations between cluster-group membership and socio-occupational functioning (using the Social and Occupational Functioning Assessment Scale) over 3 years, adjusted for gender, premorbid IQ, level of education, depressive, positive, negative and manic symptoms, and diagnosis of a primary psychotic disorder.
ResultsCluster analysis of neurocognitive test scores derived three subgroups described as ‘normal range’ (n = 243, 38.6%), ‘intermediate impairment’ (n = 252, 40.1%), and ‘global impairment’ (n = 134, 21.3%). The major mental disorder categories (depressive, anxiety, bipolar, psychotic and other) were represented in each neurocognitive subgroup. The global impairment subgroup had lower functioning for 3 years of follow-up; however, neither the global impairment (B = 0.26, 95% CI −0.67 to 1.20; P = 0.581) or intermediate impairment (B = 0.46, 95% CI −0.26 to 1.19; P = 0.211) subgroups differed from the normal range subgroup in their rate of change in functioning over time.
ConclusionsNeurocognitive impairment may follow a continuum of severity across the major syndrome-based mental disorders, with data-driven neurocognitive subgroups predictive of functional course. Of note, the global impairment subgroup had longstanding functional impairment despite continuing engagement with clinical services.
Early identification of impending cardiac arrest in neonates and infants in the cardiovascular ICU: a statistical modelling approach using physiologic monitoring data – CORRIGENDUM
- Sanjukta N. Bose, Adam Verigan, Jade Hanson, Luis M. Ahumada, Sharon R. Ghazarian, Neil A. Goldenberg, Arabela Stock, Jeffrey P. Jacobs
-
- Journal:
- Cardiology in the Young / Volume 29 / Issue 11 / November 2019
- Published online by Cambridge University Press:
- 09 October 2019, p. 1349
-
- Article
-
- You have access Access
- HTML
- Export citation
Early identification of impending cardiac arrest in neonates and infants in the cardiovascular ICU: a statistical modelling approach using physiologic monitoring data
- Sanjukta N. Bose, Adam Verigan, Jade Hanson, Luis M. Ahumada, Sharon R. Ghazarian, Neil A. Goldenberg, Arabela Stock, Jeffrey P. Jacobs
-
- Journal:
- Cardiology in the Young / Volume 29 / Issue 11 / November 2019
- Published online by Cambridge University Press:
- 09 September 2019, pp. 1340-1348
-
- Article
- Export citation
-
Objective:
To develop a physiological data-driven model for early identification of impending cardiac arrest in neonates and infants with cardiac disease hospitalised in the cardiovascular ICU.
Methods:We performed a single-institution retrospective cohort study (11 January 2013–16 September 2015) of patients ≤1 year old with cardiac disease who were hospitalised in the cardiovascular ICU at a tertiary care children’s hospital. Demographics and diagnostic codes of cardiac arrest were obtained via the electronic health record. Diagnosis of cardiac arrest was validated by expert clinician review. Minute-to-minute physiological monitoring data were recorded via bedside monitors. A generalized linear model was used to compute a minute by minute risk score. Training and test data sets both included data from patients who did and did not develop cardiac arrest. An optimal risk-score threshold was derived based on the model’s discriminatory capacity for impending arrest versus non-arrest. Model performance measures included sensitivity, specificity, accuracy, likelihood ratios, and post-test probability of arrest.
Results:The final model consisting of multiple clinical parameters was able to identify impending cardiac arrest at least 2 hours prior to the event with an overall accuracy of 75% (sensitivity = 61%, specificity = 80%) and observed an increase in probability of detection of cardiac arrest from a pre-test probability of 9.6% to a post-test probability of 21.2%.
Conclusions:Our findings demonstrate that a predictive model using physiologic monitoring data in neonates and infants with cardiac disease hospitalised in the paediatric cardiovascular ICU can identify impending cardiac arrest on average 17 hours prior to arrest.
Eighteen years of paediatric extracorporeal membrane oxygenation and ventricular assist devices: insight regarding late outcomes
- Shawn M. Shah, David W. Kays, Sharon R. Ghazarian, Tom R. Karl, Plato Alexander, Nathaniel Sznycer-Taub, Jason Parker, Molly Oldeen, Melvin C. Almodovar, Gary Stapleton, James A. Quintessenza, Alfred Asante-Korang, Vyas Kartha, Jade Hanson, Ernest Amankwah, Joeli Roth, Jeffrey P. Jacobs
-
- Journal:
- Cardiology in the Young / Volume 28 / Issue 11 / November 2018
- Published online by Cambridge University Press:
- 17 September 2018, pp. 1316-1322
-
- Article
- Export citation
-
Background
We reviewed all patients who were supported with extracorporeal membrane oxygenation and/or ventricular assist device at our institution in order to describe diagnostic characteristics and assess mortality.
MethodsA retrospective cohort study was performed including all patients supported with extracorporeal membrane oxygenation and/or ventricular assist device from our first case (8 October, 1998) through 25 July, 2016. The primary outcome of interest was mortality, which was modelled by the Kaplan–Meier method.
ResultsA total of 223 patients underwent 241 extracorporeal membrane oxygenation runs. Median support time was 4.0 days, ranging from 0.04 to 55.8 days, with a mean of 6.4±7.0 days. Mean (±SD) age at initiation was 727.4 days (±146.9 days). Indications for extracorporeal membrane oxygenation were stratified by primary indication: cardiac extracorporeal membrane oxygenation (n=175; 72.6%) or respiratory extracorporeal membrane oxygenation (n=66; 27.4%). The most frequent diagnosis for cardiac extracorporeal membrane oxygenation patients was hypoplastic left heart syndrome or hypoplastic left heart syndrome-related malformation (n=55 patients with HLHS who underwent 64 extracorporeal membrane oxygenation runs). For respiratory extracorporeal membrane oxygenation, the most frequent diagnosis was congenital diaphragmatic hernia (n=22). A total of 24 patients underwent 26 ventricular assist device runs. Median support time was 7 days, ranging from 0 to 75 days, with a mean of 15.3±18.8 days. Mean age at initiation of ventricular assist device was 2530.8±660.2 days (6.93±1.81 years). Cardiomyopathy/myocarditis was the most frequent indication for ventricular assist device placement (n=14; 53.8%). Survival to discharge was 42.2% for extracorporeal membrane oxygenation patients and 54.2% for ventricular assist device patients. Kaplan–Meier 1-year survival was as follows: all patients, 41.0%; extracorporeal membrane oxygenation patients, 41.0%; and ventricular assist device patients, 43.2%. Kaplan–Meier 5-year survival was as follows: all patients, 39.7%; extracorporeal membrane oxygenation patients, 39.7%; and ventricular assist device patients, 43.2%.
ConclusionsThis single-institutional 18-year review documents the differential probability of survival for various sub-groups of patients who require support with extracorporeal membrane oxygenation or ventricular assist device. The indication for mechanical circulatory support, underlying diagnosis, age, and setting in which cannulation occurs may affect survival after extracorporeal membrane oxygenation and ventricular assist device. The Kaplan–Meier analyses in this study demonstrate that patients who survive to hospital discharge have an excellent chance of longer-term survival.
The role of Pine Island Glacier ice shelf basal channels in deep-water upwelling, polynyas and ocean circulation in Pine Island Bay, Antarctica
- Kenneth D. Mankoff, Stanley S. Jacobs, Slawek M. Tulaczyk, Sharon E. Stammerjohn
-
- Journal:
- Annals of Glaciology / Volume 53 / Issue 60 / 2012
- Published online by Cambridge University Press:
- 14 September 2017, pp. 123-128
-
- Article
-
- You have access Access
- HTML
- Export citation
-
Several hundred visible and thermal infrared satellite images of Antarctica’s southeast Amundsen Sea from 1986 to 2011, combined with aerial observations in 2009, show a strong inverse relation between prominent curvilinear surface depressions and the underlying basal morphology of the outer Pine Island Glacier ice shelf. Shipboard measurements near the calving front reveal positive temperature, salinity and current anomalies indicative of melt-laden, deep-water outflows near and above the larger channel termini. These buoyant plumes rise to the surface and are expressed as small polynyas in the sea ice and thermal signatures in the open water. The warm upwellings also trace the cyclonic surface circulation in Pine Island Bay. The satellite coverage suggests changing modes of ocean/ice interactions, dominated by leads along the ice shelf through 1999, fast ice and polynyas from 2000 to 2007, and larger areas of open water since 2008.
Contributors
-
- By Carsten Allefeld, Silke Anders, Michael Andric, Sharon Ash, Mark Blokpoel, Giovanna Egidi, Murray Grossman, Uri Hasson, John-Dylan Haynes, Arthur M. Jacobs, Pia Knoeferle, Line Burholt Kristensen, Anna K. Kuhlen, Christopher A. Kurby, Iris van Rooij, Jeremy I. Skipper, Steven L. Small, Arjen Stolk, Ivan Toni, Mikkel Wallentin, Roel M. Willems, Jeffrey M. Zacks
- Edited by Roel M. Willems, Radboud Universiteit Nijmegen
-
- Book:
- Cognitive Neuroscience of Natural Language Use
- Published online:
- 05 February 2015
- Print publication:
- 12 February 2015, pp x-xi
-
- Chapter
- Export citation
Antarctic climate change and the environment: an update
- John Turner, Nicholas E. Barrand, Thomas J. Bracegirdle, Peter Convey, Dominic A. Hodgson, Martin Jarvis, Adrian Jenkins, Gareth Marshall, Michael P. Meredith, Howard Roscoe, Jon Shanklin, John French, Hugues Goosse, Mauro Guglielmin, Julian Gutt, Stan Jacobs, Marlon C. Kennicutt II, Valerie Masson-Delmotte, Paul Mayewski, Francisco Navarro, Sharon Robinson, Ted Scambos, Mike Sparrow, Colin Summerhayes, Kevin Speer, Alexander Klepikov
-
- Journal:
- Polar Record / Volume 50 / Issue 3 / June 2014
- Published online by Cambridge University Press:
- 18 April 2013, pp. 237-259
-
- Article
- Export citation
-
We present an update of the ‘key points’ from the Antarctic Climate Change and the Environment (ACCE) report that was published by the Scientific Committee on Antarctic Research (SCAR) in 2009. We summarise subsequent advances in knowledge concerning how the climates of the Antarctic and Southern Ocean have changed in the past, how they might change in the future, and examine the associated impacts on the marine and terrestrial biota. We also incorporate relevant material presented by SCAR to the Antarctic Treaty Consultative Meetings, and make use of emerging results that will form part of the Intergovernmental Panel on Climate Change (IPCC) Fifth Assessment Report.
Contributors
-
- By Graeme J.M. Alexander, Heung Bae Kim, Michael Burch, Andrew J. Butler, Tanveer Butt, Roy Calne, Edward Cantu, Robert B. Colvin, Paul Corris, Charles Crawley, Hiroshi Date, Francis L. Delmonico, Bimalangshu R. Dey, Kate Drummond, John Dunning, John D. Firth, John Forsythe, Simon M. Gabe, Robert S. Gaston, William Gelson, Paul Gibbs, Alex Gimson, Leo C. Ginns, Samuel Goldfarb, Ryoichi Goto, Walter K. Graham, Simon J.F. Harper, Koji Hashimoto, David G. Healy, Hassan N. Ibrahim, David Ip, Fadi G. Issa, Neville V. Jamieson, David P. Jenkins, Dixon B. Kaufman, Kiran K. Khush, Heung Bae Kim, Andrew A. Klein, John Klinck, Camille Nelson Kotton, Vineeta Kumar, Yael B. Kushner, D. Frank. P. Larkin, Clive J. Lewis, Yvonne H. Luo, Richard S. Luskin, Ernest I. Mandel, James F. Markmann, Lorna Marson, Arthur J. Matas, Mandeep R. Mehra, Stephen J. Middleton, Giorgina Mieli-Vergani, Charles Miller, Sharon Mulroy, Faruk Özalp, Can Ozturk, Jayan Parameshwar, J.S. Parmar, Hari K. Parthasarathy, Nick Pritchard, Cristiano Quintini, Axel O. Rahmel, Chris J. Rudge, Stephan V.B. Schueler, Maria Siemionow, Jacob Simmonds, Peter Slinger, Thomas R. Spitzer, Stuart C. Sweet, Nina E. Tolkoff-Rubin, Steven S.L. Tsui, Khashayar Vakili, R.V. Venkateswaran, Hector Vilca-Melendez, Vladimir Vinarsky, Kathryn J. Wood, Heidi Yeh, David W. Zaas, Jonathan G. Zaroff
- Edited by Andrew A. Klein, Clive J. Lewis, Joren C. Madsen
-
- Book:
- Organ Transplantation
- Published online:
- 07 September 2011
- Print publication:
- 11 August 2011, pp vii-x
-
- Chapter
- Export citation
Contributors
-
- By Shamsuddin Akhtar, Greg Albert, Sidney Allison, Muhammad Anwar, Haruo Arita, Amanda Barker, Mary Hanna Bekhit, Jeanna Blitz, Tyson Bolinske, David Burbulys, Asokumar Buvanendran, Gregory Cain, Keith A. Candiotti, Daniel B. Carr, Derek Chalmers, John Charney, Rex Cheng, Roger Chou, Keun Sam Chung, Anna Clebone, Frederick Conlin, Susan Dabu-Bondoc, Tiffany Denepitiya-Balicki, Jeanette Derdemezi, Anahat Kaur Dhillon, Ho Dzung, Juan Jose Egas, Stephen M. Eskaros, Zhuang T. Fang, Claudia R. Fernandez Robles, Victor A. Filadora, Ellen Flanagan, Dan Froicu, Allison Gandey, Nehal Gatha, Boris Gelman, Christopher Gharibo, Muhammad K. Ghori, Brian Ginsberg, Michael E. Goldberg, Jeff Gudin, Thomas Halaszynski, Martin Hale, Dorothea Hall, Craig T. Hartrick, Justin Hata, Lars E. Helgeson, Joe C. Hong, Richard W. Hong, Balazs Horvath, Eric S. Hsu, Gabriel Jacobs, Jonathan S. Jahr, Rongjie Jaing, Inderjeet Singh Julka, Zeev N. Kain, Clinton Kakazu, Kianusch Kiai, Mary Keyes, Michael M. Kim, Peter G. Lacouture, Ryan Lanier, Vivian K. Lee, Mark J. Lema, Oscar A. de Leon-Casasola, Imanuel Lerman, Philip Levin, Steven Levin, JinLei Li, Eric C. Lin, Sharon Lin, David A. Lindley, Ana M. Lobo, Marisa Lomanto, Mirjana Lovrincevic, Brenda C. McClain, Tariq Malik, Jure Marijic, Joseph Marino, Laura Mechtler, Alan Miller, Carly Miller, Amit Mirchandani, Sukanya Mitra, Fleurise Montecillo, James M. Moore, Debra E. Morrison, Philip F. Morway, Carsten Nadjat-Haiem, Hamid Nourmand, Dana Oprea, Sunil J. Panchal, Edward J. Park, Kathleen Ji Park, Kellie Park, Parisa Partownavid, Akta Patel, Bijal Patel, Komal D. Patel, Neesa Patel, Swati Patel, Paul M. Peloso, Danielle Perret, Anthony DePlato, Marjorie Podraza Stiegler, Despina Psillides, Mamatha Punjala, Johan Raeder, Siamak Rahman, Aziz M. Razzuk, Maggy G. Riad, Kristin L. Richards, R. Todd Rinnier, Ian W. Rodger, Joseph Rosa, Abraham Rosenbaum, Alireza Sadoughi, Veena Salgar, Leslie Schechter, Michael Seneca, Yasser F. Shaheen, James H. Shull, Elizabeth Sinatra, Raymond S. Sinatra, Neil Singla, Neil Sinha, Denis V. Snegovskikh, Dmitri Souzdalnitski, Julie Sramcik, Zoreh Steffens, Alexander Timchenko, Vadim Tokhner, Marc C. Torjman, Co T. Truong, Nalini Vadivelu, Ashley Vaughn, Anjali Vira, Eugene R. Viscusi, Dajie Wang, Shu-ming Wang, J. Michael Watkins-Pitchford, Steven J. Weisman, Ira Whitten, Bryan S. Williams, Jeremy M. Wong, Thomas Wong, Christopher Wray, Yaw Wu, Anthony T. Yarussi, Laurie Yonemoto, Bita H. Zadeh, Jill Zafar, Martha Zegarra, Keren Ziv
- Edited by Raymond S. Sinatra, Jonathan S. Jahr, University of California, Los Angeles, School of Medicine, J. Michael Watkins-Pitchford
-
- Book:
- The Essence of Analgesia and Analgesics
- Published online:
- 06 December 2010
- Print publication:
- 14 October 2010, pp xi-xviii
-
- Chapter
- Export citation
Contributors
-
- By Rose Teteki Abbey, K. C. Abraham, David Tuesday Adamo, LeRoy H. Aden, Efrain Agosto, Victor Aguilan, Gillian T. W. Ahlgren, Charanjit Kaur AjitSingh, Dorothy B E A Akoto, Giuseppe Alberigo, Daniel E. Albrecht, Ruth Albrecht, Daniel O. Aleshire, Urs Altermatt, Anand Amaladass, Michael Amaladoss, James N. Amanze, Lesley G. Anderson, Thomas C. Anderson, Victor Anderson, Hope S. Antone, María Pilar Aquino, Paula Arai, Victorio Araya Guillén, S. Wesley Ariarajah, Ellen T. Armour, Brett Gregory Armstrong, Atsuhiro Asano, Naim Stifan Ateek, Mahmoud Ayoub, John Alembillah Azumah, Mercedes L. García Bachmann, Irena Backus, J. Wayne Baker, Mieke Bal, Lewis V. Baldwin, William Barbieri, António Barbosa da Silva, David Basinger, Bolaji Olukemi Bateye, Oswald Bayer, Daniel H. Bays, Rosalie Beck, Nancy Elizabeth Bedford, Guy-Thomas Bedouelle, Chorbishop Seely Beggiani, Wolfgang Behringer, Christopher M. Bellitto, Byard Bennett, Harold V. Bennett, Teresa Berger, Miguel A. Bernad, Henley Bernard, Alan E. Bernstein, Jon L. Berquist, Johannes Beutler, Ana María Bidegain, Matthew P. Binkewicz, Jennifer Bird, Joseph Blenkinsopp, Dmytro Bondarenko, Paulo Bonfatti, Riet en Pim Bons-Storm, Jessica A. Boon, Marcus J. Borg, Mark Bosco, Peter C. Bouteneff, François Bovon, William D. Bowman, Paul S. Boyer, David Brakke, Richard E. Brantley, Marcus Braybrooke, Ian Breward, Ênio José da Costa Brito, Jewel Spears Brooker, Johannes Brosseder, Nicholas Canfield Read Brown, Robert F. Brown, Pamela K. Brubaker, Walter Brueggemann, Bishop Colin O. Buchanan, Stanley M. Burgess, Amy Nelson Burnett, J. Patout Burns, David B. Burrell, David Buttrick, James P. Byrd, Lavinia Byrne, Gerado Caetano, Marcos Caldas, Alkiviadis Calivas, William J. Callahan, Salvatore Calomino, Euan K. Cameron, William S. Campbell, Marcelo Ayres Camurça, Daniel F. Caner, Paul E. Capetz, Carlos F. Cardoza-Orlandi, Patrick W. Carey, Barbara Carvill, Hal Cauthron, Subhadra Mitra Channa, Mark D. Chapman, James H. Charlesworth, Kenneth R. Chase, Chen Zemin, Luciano Chianeque, Philip Chia Phin Yin, Francisca H. Chimhanda, Daniel Chiquete, John T. Chirban, Soobin Choi, Robert Choquette, Mita Choudhury, Gerald Christianson, John Chryssavgis, Sejong Chun, Esther Chung-Kim, Charles M. A. Clark, Elizabeth A. Clark, Sathianathan Clarke, Fred Cloud, John B. Cobb, W. Owen Cole, John A Coleman, John J. Collins, Sylvia Collins-Mayo, Paul K. Conkin, Beth A. Conklin, Sean Connolly, Demetrios J. Constantelos, Michael A. Conway, Paula M. Cooey, Austin Cooper, Michael L. Cooper-White, Pamela Cooper-White, L. William Countryman, Sérgio Coutinho, Pamela Couture, Shannon Craigo-Snell, James L. Crenshaw, David Crowner, Humberto Horacio Cucchetti, Lawrence S. Cunningham, Elizabeth Mason Currier, Emmanuel Cutrone, Mary L. Daniel, David D. Daniels, Robert Darden, Rolf Darge, Isaiah Dau, Jeffry C. Davis, Jane Dawson, Valentin Dedji, John W. de Gruchy, Paul DeHart, Wendy J. Deichmann Edwards, Miguel A. De La Torre, George E. Demacopoulos, Thomas de Mayo, Leah DeVun, Beatriz de Vasconcellos Dias, Dennis C. Dickerson, John M. Dillon, Luis Miguel Donatello, Igor Dorfmann-Lazarev, Susanna Drake, Jonathan A. Draper, N. Dreher Martin, Otto Dreydoppel, Angelyn Dries, A. J. Droge, Francis X. D'Sa, Marilyn Dunn, Nicole Wilkinson Duran, Rifaat Ebied, Mark J. Edwards, William H. Edwards, Leonard H. Ehrlich, Nancy L. Eiesland, Martin Elbel, J. Harold Ellens, Stephen Ellingson, Marvin M. Ellison, Robert Ellsberg, Jean Bethke Elshtain, Eldon Jay Epp, Peter C. Erb, Tassilo Erhardt, Maria Erling, Noel Leo Erskine, Gillian R. Evans, Virginia Fabella, Michael A. Fahey, Edward Farley, Margaret A. Farley, Wendy Farley, Robert Fastiggi, Seena Fazel, Duncan S. Ferguson, Helwar Figueroa, Paul Corby Finney, Kyriaki Karidoyanes FitzGerald, Thomas E. FitzGerald, John R. Fitzmier, Marie Therese Flanagan, Sabina Flanagan, Claude Flipo, Ronald B. Flowers, Carole Fontaine, David Ford, Mary Ford, Stephanie A. Ford, Jim Forest, William Franke, Robert M. Franklin, Ruth Franzén, Edward H. Friedman, Samuel Frouisou, Lorelei F. Fuchs, Jojo M. Fung, Inger Furseth, Richard R. Gaillardetz, Brandon Gallaher, China Galland, Mark Galli, Ismael García, Tharscisse Gatwa, Jean-Marie Gaudeul, Luis María Gavilanes del Castillo, Pavel L. Gavrilyuk, Volney P. Gay, Metropolitan Athanasios Geevargis, Kondothra M. George, Mary Gerhart, Simon Gikandi, Maurice Gilbert, Michael J. Gillgannon, Verónica Giménez Beliveau, Terryl Givens, Beth Glazier-McDonald, Philip Gleason, Menghun Goh, Brian Golding, Bishop Hilario M. Gomez, Michelle A. Gonzalez, Donald K. Gorrell, Roy Gottfried, Tamara Grdzelidze, Joel B. Green, Niels Henrik Gregersen, Cristina Grenholm, Herbert Griffiths, Eric W. Gritsch, Erich S. Gruen, Christoffer H. Grundmann, Paul H. Gundani, Jon P. Gunnemann, Petre Guran, Vidar L. Haanes, Jeremiah M. Hackett, Getatchew Haile, Douglas John Hall, Nicholas Hammond, Daphne Hampson, Jehu J. Hanciles, Barry Hankins, Jennifer Haraguchi, Stanley S. Harakas, Anthony John Harding, Conrad L. Harkins, J. William Harmless, Marjory Harper, Amir Harrak, Joel F. Harrington, Mark W. Harris, Susan Ashbrook Harvey, Van A. Harvey, R. Chris Hassel, Jione Havea, Daniel Hawk, Diana L. Hayes, Leslie Hayes, Priscilla Hayner, S. Mark Heim, Simo Heininen, Richard P. Heitzenrater, Eila Helander, David Hempton, Scott H. Hendrix, Jan-Olav Henriksen, Gina Hens-Piazza, Carter Heyward, Nicholas J. Higham, David Hilliard, Norman A. Hjelm, Peter C. Hodgson, Arthur Holder, M. Jan Holton, Dwight N. Hopkins, Ronnie Po-chia Hsia, Po-Ho Huang, James Hudnut-Beumler, Jennifer S. Hughes, Leonard M. Hummel, Mary E. Hunt, Laennec Hurbon, Mark Hutchinson, Susan E. Hylen, Mary Beth Ingham, H. Larry Ingle, Dale T. Irvin, Jon Isaak, Paul John Isaak, Ada María Isasi-Díaz, Hans Raun Iversen, Margaret C. Jacob, Arthur James, Maria Jansdotter-Samuelsson, David Jasper, Werner G. Jeanrond, Renée Jeffery, David Lyle Jeffrey, Theodore W. Jennings, David H. Jensen, Robin Margaret Jensen, David Jobling, Dale A. Johnson, Elizabeth A. Johnson, Maxwell E. Johnson, Sarah Johnson, Mark D. Johnston, F. Stanley Jones, James William Jones, John R. Jones, Alissa Jones Nelson, Inge Jonsson, Jan Joosten, Elizabeth Judd, Mulambya Peggy Kabonde, Robert Kaggwa, Sylvester Kahakwa, Isaac Kalimi, Ogbu U. Kalu, Eunice Kamaara, Wayne C. Kannaday, Musimbi Kanyoro, Veli-Matti Kärkkäinen, Frank Kaufmann, Léon Nguapitshi Kayongo, Richard Kearney, Alice A. Keefe, Ralph Keen, Catherine Keller, Anthony J. Kelly, Karen Kennelly, Kathi Lynn Kern, Fergus Kerr, Edward Kessler, George Kilcourse, Heup Young Kim, Kim Sung-Hae, Kim Yong-Bock, Kim Yung Suk, Richard King, Thomas M. King, Robert M. Kingdon, Ross Kinsler, Hans G. Kippenberg, Cheryl A. Kirk-Duggan, Clifton Kirkpatrick, Leonid Kishkovsky, Nadieszda Kizenko, Jeffrey Klaiber, Hans-Josef Klauck, Sidney Knight, Samuel Kobia, Robert Kolb, Karla Ann Koll, Heikki Kotila, Donald Kraybill, Philip D. W. Krey, Yves Krumenacker, Jeffrey Kah-Jin Kuan, Simanga R. Kumalo, Peter Kuzmic, Simon Shui-Man Kwan, Kwok Pui-lan, André LaCocque, Stephen E. Lahey, John Tsz Pang Lai, Emiel Lamberts, Armando Lampe, Craig Lampe, Beverly J. Lanzetta, Eve LaPlante, Lizette Larson-Miller, Ariel Bybee Laughton, Leonard Lawlor, Bentley Layton, Robin A. Leaver, Karen Lebacqz, Archie Chi Chung Lee, Marilyn J. Legge, Hervé LeGrand, D. L. LeMahieu, Raymond Lemieux, Bill J. Leonard, Ellen M. Leonard, Outi Leppä, Jean Lesaulnier, Nantawan Boonprasat Lewis, Henrietta Leyser, Alexei Lidov, Bernard Lightman, Paul Chang-Ha Lim, Carter Lindberg, Mark R. Lindsay, James R. Linville, James C. Livingston, Ann Loades, David Loades, Jean-Claude Loba-Mkole, Lo Lung Kwong, Wati Longchar, Eleazar López, David W. Lotz, Andrew Louth, Robin W. Lovin, William Luis, Frank D. Macchia, Diarmaid N. J. MacCulloch, Kirk R. MacGregor, Marjory A. MacLean, Donald MacLeod, Tomas S. Maddela, Inge Mager, Laurenti Magesa, David G. Maillu, Fortunato Mallimaci, Philip Mamalakis, Kä Mana, Ukachukwu Chris Manus, Herbert Robinson Marbury, Reuel Norman Marigza, Jacqueline Mariña, Antti Marjanen, Luiz C. L. Marques, Madipoane Masenya (ngwan'a Mphahlele), Caleb J. D. Maskell, Steve Mason, Thomas Massaro, Fernando Matamoros Ponce, András Máté-Tóth, Odair Pedroso Mateus, Dinis Matsolo, Fumitaka Matsuoka, John D'Arcy May, Yelena Mazour-Matusevich, Theodore Mbazumutima, John S. McClure, Christian McConnell, Lee Martin McDonald, Gary B. McGee, Thomas McGowan, Alister E. McGrath, Richard J. McGregor, John A. McGuckin, Maud Burnett McInerney, Elsie Anne McKee, Mary B. McKinley, James F. McMillan, Ernan McMullin, Kathleen E. McVey, M. Douglas Meeks, Monica Jyotsna Melanchthon, Ilie Melniciuc-Puica, Everett Mendoza, Raymond A. Mentzer, William W. Menzies, Ina Merdjanova, Franziska Metzger, Constant J. Mews, Marvin Meyer, Carol Meyers, Vasile Mihoc, Gunner Bjerg Mikkelsen, Maria Inêz de Castro Millen, Clyde Lee Miller, Bonnie J. Miller-McLemore, Alexander Mirkovic, Paul Misner, Nozomu Miyahira, R. W. L. Moberly, Gerald Moede, Aloo Osotsi Mojola, Sunanda Mongia, Rebeca Montemayor, James Moore, Roger E. Moore, Craig E. Morrison O.Carm, Jeffry H. Morrison, Keith Morrison, Wilson J. Moses, Tefetso Henry Mothibe, Mokgethi Motlhabi, Fulata Moyo, Henry Mugabe, Jesse Ndwiga Kanyua Mugambi, Peggy Mulambya-Kabonde, Robert Bruce Mullin, Pamela Mullins Reaves, Saskia Murk Jansen, Heleen L. Murre-Van den Berg, Augustine Musopole, Isaac M. T. Mwase, Philomena Mwaura, Cecilia Nahnfeldt, Anne Nasimiyu Wasike, Carmiña Navia Velasco, Thulani Ndlazi, Alexander Negrov, James B. Nelson, David G. Newcombe, Carol Newsom, Helen J. Nicholson, George W. E. Nickelsburg, Tatyana Nikolskaya, Damayanthi M. A. Niles, Bertil Nilsson, Nyambura Njoroge, Fidelis Nkomazana, Mary Beth Norton, Christian Nottmeier, Sonene Nyawo, Anthère Nzabatsinda, Edward T. Oakes, Gerald O'Collins, Daniel O'Connell, David W. Odell-Scott, Mercy Amba Oduyoye, Kathleen O'Grady, Oyeronke Olajubu, Thomas O'Loughlin, Dennis T. Olson, J. Steven O'Malley, Cephas N. Omenyo, Muriel Orevillo-Montenegro, César Augusto Ornellas Ramos, Agbonkhianmeghe E. Orobator, Kenan B. Osborne, Carolyn Osiek, Javier Otaola Montagne, Douglas F. Ottati, Anna May Say Pa, Irina Paert, Jerry G. Pankhurst, Aristotle Papanikolaou, Samuele F. Pardini, Stefano Parenti, Peter Paris, Sung Bae Park, Cristián G. Parker, Raquel Pastor, Joseph Pathrapankal, Daniel Patte, W. Brown Patterson, Clive Pearson, Keith F. Pecklers, Nancy Cardoso Pereira, David Horace Perkins, Pheme Perkins, Edward N. Peters, Rebecca Todd Peters, Bishop Yeznik Petrossian, Raymond Pfister, Peter C. Phan, Isabel Apawo Phiri, William S. F. Pickering, Derrick G. Pitard, William Elvis Plata, Zlatko Plese, John Plummer, James Newton Poling, Ronald Popivchak, Andrew Porter, Ute Possekel, James M. Powell, Enos Das Pradhan, Devadasan Premnath, Jaime Adrían Prieto Valladares, Anne Primavesi, Randall Prior, María Alicia Puente Lutteroth, Eduardo Guzmão Quadros, Albert Rabil, Laurent William Ramambason, Apolonio M. Ranche, Vololona Randriamanantena Andriamitandrina, Lawrence R. Rast, Paul L. Redditt, Adele Reinhartz, Rolf Rendtorff, Pål Repstad, James N. Rhodes, John K. Riches, Joerg Rieger, Sharon H. Ringe, Sandra Rios, Tyler Roberts, David M. Robinson, James M. Robinson, Joanne Maguire Robinson, Richard A. H. Robinson, Roy R. Robson, Jack B. Rogers, Maria Roginska, Sidney Rooy, Rev. Garnett Roper, Maria José Fontelas Rosado-Nunes, Andrew C. Ross, Stefan Rossbach, François Rossier, John D. Roth, John K. Roth, Phillip Rothwell, Richard E. Rubenstein, Rosemary Radford Ruether, Markku Ruotsila, John E. Rybolt, Risto Saarinen, John Saillant, Juan Sanchez, Wagner Lopes Sanchez, Hugo N. Santos, Gerhard Sauter, Gloria L. Schaab, Sandra M. Schneiders, Quentin J. Schultze, Fernando F. Segovia, Turid Karlsen Seim, Carsten Selch Jensen, Alan P. F. Sell, Frank C. Senn, Kent Davis Sensenig, Damían Setton, Bal Krishna Sharma, Carolyn J. Sharp, Thomas Sheehan, N. Gerald Shenk, Christian Sheppard, Charles Sherlock, Tabona Shoko, Walter B. Shurden, Marguerite Shuster, B. Mark Sietsema, Batara Sihombing, Neil Silberman, Clodomiro Siller, Samuel Silva-Gotay, Heikki Silvet, John K. Simmons, Hagith Sivan, James C. Skedros, Abraham Smith, Ashley A. Smith, Ted A. Smith, Daud Soesilo, Pia Søltoft, Choan-Seng (C. S.) Song, Kathryn Spink, Bryan Spinks, Eric O. Springsted, Nicolas Standaert, Brian Stanley, Glen H. Stassen, Karel Steenbrink, Stephen J. Stein, Andrea Sterk, Gregory E. Sterling, Columba Stewart, Jacques Stewart, Robert B. Stewart, Cynthia Stokes Brown, Ken Stone, Anne Stott, Elizabeth Stuart, Monya Stubbs, Marjorie Hewitt Suchocki, David Kwang-sun Suh, Scott W. Sunquist, Keith Suter, Douglas Sweeney, Charles H. Talbert, Shawqi N. Talia, Elsa Tamez, Joseph B. Tamney, Jonathan Y. Tan, Yak-Hwee Tan, Kathryn Tanner, Feiya Tao, Elizabeth S. Tapia, Aquiline Tarimo, Claire Taylor, Mark Lewis Taylor, Bishop Abba Samuel Wolde Tekestebirhan, Eugene TeSelle, M. Thomas Thangaraj, David R. Thomas, Andrew Thornley, Scott Thumma, Marcelo Timotheo da Costa, George E. “Tink” Tinker, Ola Tjørhom, Karen Jo Torjesen, Iain R. Torrance, Fernando Torres-Londoño, Archbishop Demetrios [Trakatellis], Marit Trelstad, Christine Trevett, Phyllis Trible, Johannes Tromp, Paul Turner, Robert G. Tuttle, Archbishop Desmond Tutu, Peter Tyler, Anders Tyrberg, Justin Ukpong, Javier Ulloa, Camillus Umoh, Kristi Upson-Saia, Martina Urban, Monica Uribe, Elochukwu Eugene Uzukwu, Richard Vaggione, Gabriel Vahanian, Paul Valliere, T. J. Van Bavel, Steven Vanderputten, Peter Van der Veer, Huub Van de Sandt, Louis Van Tongeren, Luke A. Veronis, Noel Villalba, Ramón Vinke, Tim Vivian, David Voas, Elena Volkova, Katharina von Kellenbach, Elina Vuola, Timothy Wadkins, Elaine M. Wainwright, Randi Jones Walker, Dewey D. Wallace, Jerry Walls, Michael J. Walsh, Philip Walters, Janet Walton, Jonathan L. Walton, Wang Xiaochao, Patricia A. Ward, David Harrington Watt, Herold D. Weiss, Laurence L. Welborn, Sharon D. Welch, Timothy Wengert, Traci C. West, Merold Westphal, David Wetherell, Barbara Wheeler, Carolinne White, Jean-Paul Wiest, Frans Wijsen, Terry L. Wilder, Felix Wilfred, Rebecca Wilkin, Daniel H. Williams, D. Newell Williams, Michael A. Williams, Vincent L. Wimbush, Gabriele Winkler, Anders Winroth, Lauri Emílio Wirth, James A. Wiseman, Ebba Witt-Brattström, Teofil Wojciechowski, John Wolffe, Kenman L. Wong, Wong Wai Ching, Linda Woodhead, Wendy M. Wright, Rose Wu, Keith E. Yandell, Gale A. Yee, Viktor Yelensky, Yeo Khiok-Khng, Gustav K. K. Yeung, Angela Yiu, Amos Yong, Yong Ting Jin, You Bin, Youhanna Nessim Youssef, Eliana Yunes, Robert Michael Zaller, Valarie H. Ziegler, Barbara Brown Zikmund, Joyce Ann Zimmerman, Aurora Zlotnik, Zhuo Xinping
- Edited by Daniel Patte, Vanderbilt University, Tennessee
-
- Book:
- The Cambridge Dictionary of Christianity
- Published online:
- 05 August 2012
- Print publication:
- 20 September 2010, pp xi-xliv
-
- Chapter
- Export citation
Recent Developments in Health Law
- Paul Bailin, Elizabeth Gerber, Sharon Jacobs
-
- Journal:
- Journal of Law, Medicine & Ethics / Volume 36 / Issue 2 / Summer 2008
- Published online by Cambridge University Press:
- 01 January 2021, pp. 425-434
- Print publication:
- Summer 2008
-
- Article
- Export citation
On the Mend: The Ninth Circuit Gives San Francisco’s Health Care Security Ordinance the Green Light (For Now)
- Sharon Jacobs
-
- Journal:
- Journal of Law, Medicine & Ethics / Volume 36 / Issue 2 / Summer 2008
- Published online by Cambridge University Press:
- 01 January 2021, pp. 431-434
- Print publication:
- Summer 2008
-
- Article
- Export citation
-
If Justice Louis Brandeis were alive to witness San Francisco’s recent experiment with universal health care legislation, he might amend his famous characterization of the states as “laboratories of democracy” to include municipalities as well. In San Francisco, where ten percent of residents have no health insurance and where fifteen percent of businesses provide no health coverage for their employees, the Board of Supervisors recently passed the San Francisco Health Care Security Ordinance (Ordinance), which funds a network of primary care services for uninsured residents. While the Ordinance has, in the main, met with general approval, its provision mandating contributions from local businesses that do not meet minimum health spending requirements is the subject of ongoing litigation. The Ninth Circuit Court of Appeals recently ruled in the city’s favor, thereby allowing the spending provision to go forward pending a full appeal on the merits of the case.
Methicillin-Resistant Staphylococcus aureus in the Community: A Hospital-Based Study
- Angella Goetz, Kathy Posey, Jean Fleming, Sharon Jacobs, Linda Boody, Marilyn M. Wagener, Robert R. Muder
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 20 / Issue 10 / October 1999
- Published online by Cambridge University Press:
- 02 January 2015, pp. 689-691
- Print publication:
- October 1999
-
- Article
- Export citation
-
To determine the proportion of methicillin-resistant Staphylococcus aureus (MRSA) among patients presenting for hospitalization and to assess risk factors for MRSA carriage, we conducted a study for 13 months at five Pittsburgh-area hospitals. Of 504 S aureus identified, 125 (25%) were MRSA Independent risk factors for MRSA included organ transplantation, employment in a healthcare facility, pressure sores, tube feeding, and hospitalization within the preceding year.






